Is mixing prescription medication and marijuana safe?
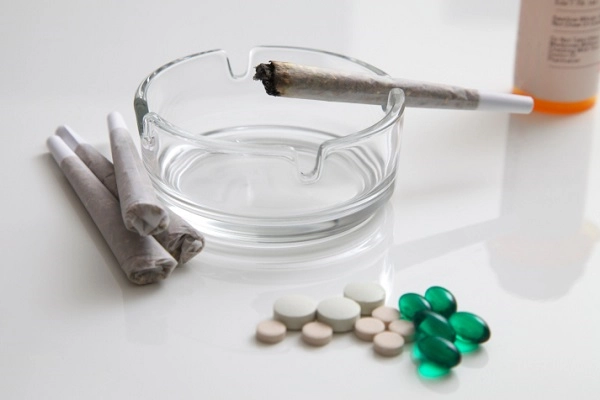

Now that recreational marijuana is legal in Oregon, questions about its interactions with prescription medications are surfacing more openly.
The answers aren’t that simple — largely due to lack of research. If you do an internet search, chances are you’ll get attacked from every direction, from the danger it poses to teenage brains, to healthier cancer treatments and miracle disease cures.
To help wade through the uncertainty, the Oregon Poison Center at Oregon Health & Science University and Salem Health have some good advice: Ask your pharmacist and/or doctor. A pharmacist knows where to look for the best drug interaction data, and can often look that information up for you on the spot.
Major research lacking
If you’re curious about pot’s long-term effect on health, heed another warning: valid research is lacking.
“Drug companies are the main research funders because they’re exploring medications they want to patent,” said Matt Tanner, Salem Health clinical pharmacy coordinator. “Until now, very little large-scale or FDA-approved work has been conducted on marijuana because it’s classified as a Schedule 1 illegal drug.”
But there’s hope that research will go forward: An article published in the February 2016 issue of JAMA Psychiatry urges, “We should try to learn as much and as rapidly as we can from the ongoing changes in local policies to minimize the harms and maximize the potential benefits.”
Some effects are well-known
THC — the active ingredient in marijuana — is a highly “protein binding” substance, meaning it attaches to plasma proteins in the blood. This means it could displace other protein-bound drugs (examples include anticoagulants like warfarin, listed in the examples below) and cause unexpected side effects.
Sources of the following include the OPC, Salem Health and the Mayo Clinic:
- Marijuana’s biggest-known impact is with opioids (for pain), sleep medications, muscle relaxants and alcohol because all affect the central nervous system. Taken with marijuana, one tends to amplify the other, Tanner said. Rob Hendrickson, MD, associate medical director of the Oregon Poison Center, also agreed that marijuana used with sedatives and hypnotics can have an additive effect.
- Marijuana may increase the risk of bleeding when taken with drugs that increase the risk of bleeding. Some examples include aspirin, anticoagulants (blood thinners) such as warfarin (Coumadin®) or heparin, antiplatelet drugs such as clopidogrel (Plavix®), and nonsteroidal anti-inflammatory drugs such as ibuprofen (Motrin®, Advil®) or naproxen (Naprosyn®, Aleve®).
- Marijuana may affect blood sugar levels. Caution is advised when using medications that may affect blood sugar. People taking medication or insulin for diabetes should be monitored closely by a qualified health care professional, including a pharmacist. Medication adjustments may be necessary.
- Marijuana may cause low blood pressure. Caution is advised in people taking drugs that lower blood pressure.
One bit of research is certain, however: THC levels in today's pot are higher, so its effect is stronger. In the 1980s, THC content averaged 4 percent; now it’s close to 10 percent and expected to plateau at 15 to 16 percent. (The federal government studies THC levels from confiscated pot.)
Prepare to wade through a quagmire of contradictions in your own research. For example, some sites say research has been suppressed. Others will cite amazing cures, from blindness to cancer. Read respected, unbiased, peer-reviewed information not promoted by special interests, which include both marijuana and pharmaceutical industries. The OPC and Salem Health recommend MedlinePlus and WebMD.
Finally, remember this safety tip: If, after checking in with your doctor or pharmacist, you’ve decided to use marijuana and suspect a possible overdose or adverse reaction, you should call the Oregon Poison Center immediately at 800-222-1222.
Keep the number in your contacts list — also on your fridge … since you may be opening that door quite often anyway.